Despite funding cuts, an AIDS ministry founded by Maryknoll continues to provide hope in the slums of Nairobi.
Florence Mwikani navigates the narrow passageways of Nairobi’s sprawling Mathare slum on a sacred mission: to keep people alive.
For 33 years, Mwikani has accompanied people living with HIV, first consoling them as they succumbed to the virus, then encouraging them as modern medications allowed them to go on living.
Now she faces a new challenge. Funding cuts last year abruptly gutted the budgets of AIDS programs around the world.
Mwikani has been a community healthcare worker for the Eastern Deanery AIDS Relief Program (EDARP) since 1993, when Maryknoll Father Edward Phillips asked Catholic churches in the eastern slums of Nairobi to recommend volunteers. Few came forward because of the fear and stigma associated with HIV.
Yet when she heard the appeal in a meeting of her small Christian community, Mwikani says she jumped at the chance. “I wanted to be Christ’s hands and feet in my community,” she says.
In their meager homes constructed from scrap lumber and rusting metal sheets, Mwikani nursed her patients when they fell ill. At times she carried them on her back to the nearby EDARP clinic. She and other outreach workers were often seen as harbingers of death. Sometimes neighbors refused to answer when she knocked on their doors.
But then came antiretroviral medications, a pharmaceutical reprieve that suppressed levels of the virus in the body and allowed countless HIV-positive people to live relatively normal lives. Mwikani’s role changed. She became a coach, making sure her patients stayed on their meds, while also assuring that their other needs in the slum were met.
Although her destitute patients had access to life-saving drugs, they often lacked sufficient food. As part of EDARP’s commitment to the overall well-being of its patients, Mwikani provided nutritional assistance.
She also provided special care for pregnant women both before and after birth. By assuring that pregnant women stay on medication, EDARP has prevented mother-to-child transmission of the virus in over 98 percent of births in recent years.
Tuberculosis is endemic in Kenya and is the leading cause of death for people with HIV. As a result, EDARP integrated TB detection and treatment into its HIV programming, becoming an international model for treating the two diseases together.

Alice Njoroge, managing director of the Eastern Deanery AIDS Relief Program, speaks with a client. Njoroge says that eight of EDARP’s 14 clinics closed due to funding cuts. (Paul Jeffrey/Kenya)
When no other funding source was available, the Maryknoll Society often stepped in to fund EDARP’s services, such as a screening program for cervical cancer — which HIV-positive women are about six times more likely to develop.
Father Phillips says that EDARP has always been about more than simply providing clinical treatment for disease.
“From our inception, we’ve been based in the slums where the poorest of the poor live,” he says. “From the beginning we offered a warm welcome to anyone seeking our help, as Jesus welcomed the lepers and blind.”
When Stacy Adhiambo learned she was HIV positive at the age of 15, it felt like the end of the world. But Josephine Kamau, an EDARP community healthcare worker, convinced her not to give up.
“I felt like killing myself when they told me I was HIV positive,” says Adhiambo, now 26. “But thank God for Josephine. She told me how important the drugs were, the reasons for me to take them. Because of her, I am still alive.”
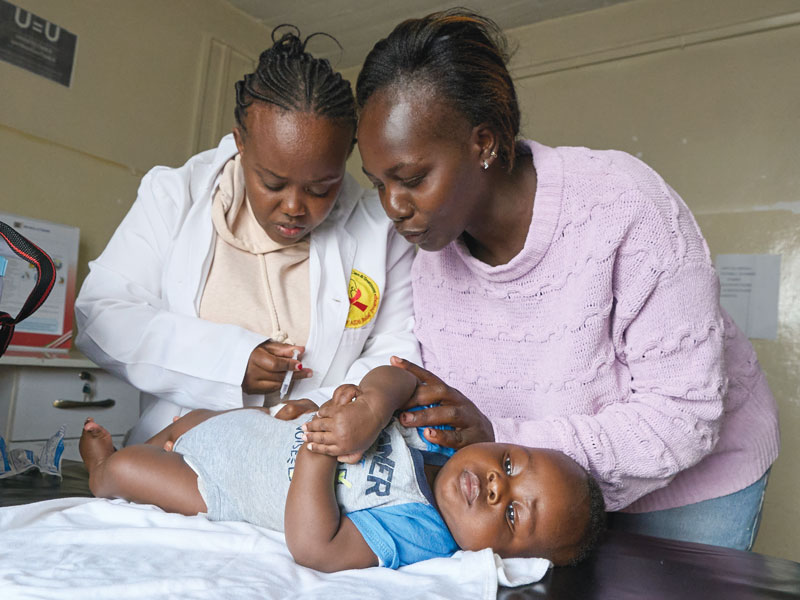
Nurse Mary Kamau vaccinates the child of an HIV-positive mother. Thanks to EDARP, transmission of the virus to all four of this mother’s children has been prevented. (Paul Jeffrey/Kenya)
EDARP employs 46 HIV-positive peer mentors for additional support. Having themselves gone through diagnosis and treatment, they counsel newly diagnosed patients.
Maureen Mauti is one of them. She says the main thing that peer mentors provide is hope.
“People often feel hopeless when they learn their status, but when you tell them your story, they gain hope that they can survive,” she says.
As the health of older adults living with HIV in the slums of Nairobi stabilized, EDARP’s managing director, Alice Njoroge, saw another need. The organization aims to reach younger people, who suffer higher rates of new infections and lower rates of compliance with antiretroviral therapy. Njoroge says EDARP recently began partnering with private pharmacies.
“A lot of adolescents will go to the pharmacies rather than come to the clinics. They go there, they buy their medication and that’s it,” she says. “We’ve worked with the pharmacies so they will refer them to us.”
Of the 1.4 million people in Kenya living with HIV, 1.3 million are on antiretroviral therapy, and the availability of medications and services remains critically important. In partnership with international organizations and local groups such as EDARP, the Kenyan government was moving towards fully managing and funding the national HIV response by the year 2030.

Josephine Kamau visits Stacy Adhiambo and 1-year-old Byalian at their home in the Mathare slum. Adhiambo was born HIV positive but didn’t learn her status until 2005. She started on antiretroviral treatment, which later enabled her son to be born without the virus. (Paul Jeffrey/Kenya)
Njoroge says that EDARP was already working toward ways to sustain itself in the coming years. What it wasn’t prepared for, she says, was the abrupt end to U.S. support when President Donald Trump — on his first day in office — issued an emergency stop-work order for all U.S.-funded humanitarian work around the world.
With thousands of lives at stake, EDARP staff and volunteers weren’t willing to stop their ministry. Although a memo went out immediately to all staff giving official notice of layoffs, about 95 percent of EDARP staff showed up for work the next day, despite knowing they wouldn’t be paid.
News of the stop-work order spread quickly, provoking panic.
“Patients were desperate, some of them were saying they’re going to stop their medications,” Njoroge says. “And some patients who had just begun treatment were saying, ‘Why should I continue this medication if you’re not sure that it’s going to be there?’
“I told them, ‘We still have medications. Please continue taking your medicine,’” she says. “Our role was to reassure them, although we didn’t know ourselves what was going to happen.”
Although some funding resumed after a few weeks, EDARP has struggled to keep delivering services. Last year, the organization’s annual budget shrank from $3.7 million to $2.2 million. Vital funding continues to come from the Maryknoll Fathers and Brothers, as well as other Church sources, pharmaceutical companies, and the U.S. Centers for Disease Control and Prevention.
Of approximately 400 EDARP staff at the beginning of 2025, only 191 were still employed at year’s end. Eight of EDARP’s 14 clinics — more than half — were forced to close.
Many of EDARP’s 1,537 community healthcare workers were receiving a stipend of $20 a month, but in October, those stipends ceased. Nonetheless, the volunteers continue serving their neighbors.
“It’s a calling,” says Josephine Kamau, who with other community healthcare workers was formally commissioned for the role during a Mass in her parish. “We have a heart for serving our patients.”
Njoroge says EDARP’s staff and volunteers will continue to dispense hope.
“People follow closely what is going on in the U.S. So, whatever happens there, they come to us and ask how it impacts their lives and the medicines they take. We keep reassuring them that we won’t abandon them,” Njoroge says.
“I was there when they were dying, when we had nothing. I can’t keep from worrying that we may have to witness the same thing again.”
Featured image: Florence Mwikani walks in the Mathare slum in Nairobi, where she serves as a community healthcare worker for AIDS patients. (Paul Jeffrey/Kenya)

